Two pioneering researchers have been awarded the $3 million Breakthrough Prize in Life Sciences for their foundational work in gene editing. Dr. Swee Lay Thein of the National Heart, Lung, and Blood Institute (NHLBI) and Dr. Stuart H. Orkin of Harvard University have been recognized for the basic research that paved the way for Casgevy, the first approved therapy using CRISPR technology to treat sickle cell disease and beta-thalassemia.
The Science of “Repressing the Repressor”
The path to this medical milestone began with a fundamental question: Why do some patients with blood disorders experience much milder symptoms than others?
For decades, scientists observed a biological phenomenon involving hemoglobin—the molecule in red blood cells responsible for carrying oxygen. Humans produce two main types:
1. Fetal hemoglobin: Produced in the womb.
2. Adult hemoglobin: Takes over after birth.
In most people, the body “switches off” the production of fetal hemoglobin as they mature. However, Dr. Thein’s research into large family lineages revealed that some individuals possessed a genetic quirk that allowed them to continue producing high levels of fetal hemoglobin throughout their lives.
Through detailed genetic analysis, her team identified a specific gene on chromosome 11 called BCL11A. This gene acts as a “repressor”—its job is to turn off fetal hemoglobin production. Dr. Orkin’s research proved that by using gene-editing tools to target and disable this repressor, scientists could essentially “trick” the body into keeping its fetal hemoglobin production active.
From Genetic Discovery to a “Functional Cure”
The application of this discovery led to the development of Casgevy, a treatment that utilizes CRISPR “molecular scissors” to edit a patient’s own cells. The process is highly sophisticated:
– Extraction: Bone marrow stem cells are removed from the patient.
– Editing: CRISPR is used to snip out the BCL11A repressor region.
– Reinfusion: The edited cells are infused back into the patient, where they begin producing healthy, oxygen-carrying red blood cells.
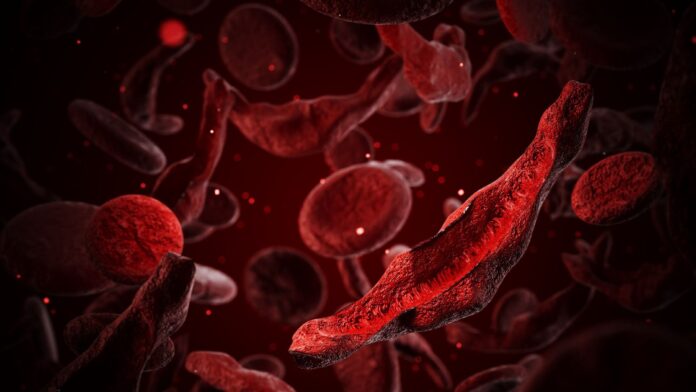
For patients with sickle cell disease—which affects 7 to 8 million people globally—this is a transformative development. In sickle cell disease, red blood cells deform into crescent shapes, causing excruciating pain, organ damage, and life-threatening blockages. By restoring fetal hemoglobin, Casgevy provides what is described as a “functional cure.”
Challenges: Accessibility and the Road Ahead
Despite the scientific triumph, the current implementation of CRISPR therapy faces significant hurdles that prevent it from being a universal solution.
1. The Physical and Financial Toll
The treatment process is incredibly taxing. Patients must undergo harsh chemotherapy to prepare their bone marrow for the new cells, a process that can take up to a year. Furthermore, the cost of the therapy runs into millions of dollars, making it inaccessible to much of the global population.
2. The Geographic Gap
Sickle cell disease and beta-thalassemia are most prevalent in Africa, Asia, and the Mediterranean—regions that often lack the high-tech medical infrastructure required for complex bone marrow transplants and gene editing.
3. The Search for Simpler Solutions
To bridge this gap, the scientific community is looking toward two main frontiers:
– “In vivo” editing: Developing methods to inject gene-editing machinery directly into the patient, eliminating the need for bone marrow extraction and reinfusion.
– Pharmacological alternatives: Researching drugs like Mitavipat, which aims to improve the metabolic health of red blood cells, potentially offering a much cheaper and more easily administered option via pills or infusions.
The Breakthrough Prize recognizes a monumental leap in genetic medicine, yet the next great challenge lies in making these life-saving technologies accessible and affordable to the millions who need them most.
Conclusion
While the recognition of Dr. Thein and Dr. Orkin marks a historic victory for gene editing, the medical community’s focus is now shifting from proving the science to solving the logistical and economic barriers of global healthcare delivery.